Living with gout or the fear of a painful flare can be frustrating. If you have ever been woken by a throbbing, red, and tender joint, you know how much it can interrupt sleep, work, and the simple joys of walking or gardening. Many people want a quick way to remove uric acid crystals and stop the pain. While there is no instant switch that dissolves crystals overnight, there are reliable, well-tested steps that can help calm a flare sooner, protect your joints, and lower uric acid over time so future attacks become less likely. Think of it as a two-part plan: soothing the pain now and steadily lowering uric acid so crystals do not build up again.
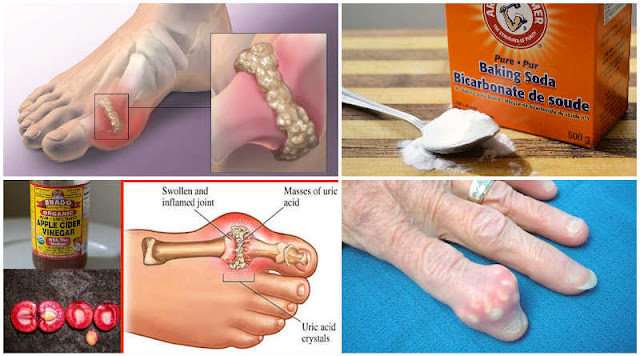
Understanding uric acid and your joints
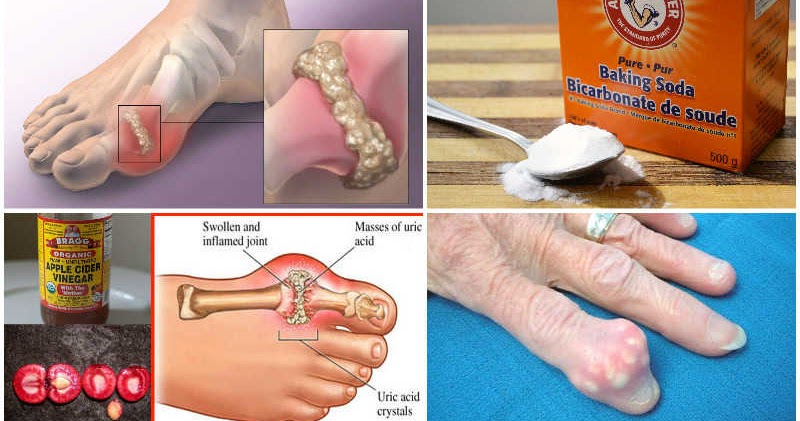
Uric acid is a natural waste product your body makes when it breaks down substances called purines. Purines are found in your own cells and in many foods. Normally, your kidneys filter uric acid and pass it out in urine. When uric acid builds up above a certain level in the blood, it can form tiny needle-like crystals that settle in joints and surrounding tissues. These crystals can trigger the intense inflammation that causes gout pain, swelling, redness, and heat. The big toe is a common place for a flare, but other joints, like the ankle, knee, and wrist, can be involved too.
It helps to remember that crystals often form quietly over time. A flare happens when your immune system reacts strongly to those crystals. In the short term, your goals are to calm the inflammation and protect the joint. In the long term, your goals are to keep uric acid low enough that crystals dissolve gradually and new ones do not form. With steady care, many people experience far fewer flares and more comfortable movement.
Can crystals be removed quickly?
It is understandable to hope for a fast fix. The truth is that crystal deposits do not disappear in a day. However, you can reduce pain and swelling quickly with the right flare care, and you can begin lowering uric acid so the body can slowly dissolve stored crystals over weeks to months. This approach is the safest and most reliable way to protect your joints.
During a flare, many people benefit from anti-inflammatory treatment discussed with a healthcare professional. Between flares, a plan to lower uric acid—through daily habits and, when needed, prescription medicines—helps prevent new crystals and encourages old ones to melt away over time. It is a marathon rather than a sprint, but most people feel the difference within a few months of consistent care.
What to do during a painful gout flare
If a joint suddenly becomes very painful, warm, red, and swollen, rest it as much as possible. Elevating the joint on pillows and applying a cool compress can bring some relief. Try to avoid putting weight on a painful foot or ankle until the inflammation starts to settle. Gentle cooling for short periods can be soothing, as long as you protect your skin with a thin cloth and avoid extreme cold.
Hydration is especially important during a flare. Sipping water regularly helps your kidneys do their job. If you use over-the-counter pain relievers, follow the label carefully and talk with your healthcare professional or pharmacist, especially if you take blood thinners or have stomach, kidney, or heart conditions. If you suspect gout and have never been diagnosed, or if the pain is severe, contact your clinician. There are effective prescription options—such as certain anti-inflammatories, colchicine, or short courses of steroids—that can shorten a flare when used appropriately. Avoid starting or stopping long-term uric acid–lowering medicines during a flare unless your clinician has advised you to do so.
Hydration: a simple daily habit that helps
Staying well hydrated helps your body flush uric acid and supports kidney health. Aim to drink water throughout the day rather than all at once. Many people find it helpful to start the morning with a glass of water and to keep a bottle nearby to sip every hour or two. If plain water is unappealing, try adding a slice of lemon or a splash of sparkling water. Unless your clinician has told you to limit fluids, steady hydration is a gentle, reliable way to support lower uric acid levels over time.
Eating in a way that supports lower uric acid
Food can play a helpful supporting role. You do not need a perfect diet, but a few steady changes make a real difference. Limiting foods that are very high in purines can reduce uric acid. These include organ meats such as liver, sweetbreads, and kidney. Some fish and shellfish, including anchovies, sardines, mussels, and herring, can also be higher in purines. Enjoying them less often, and in smaller portions, can be helpful if you are prone to gout.
Choosing lean proteins such as skinless poultry, eggs, tofu, or beans in moderate amounts can fit well into most routines. Many vegetables are excellent for health and are safe even if they contain purines, because plant purines do not have the same gout effect as certain animal sources. Filling your plate with colorful vegetables, whole grains like oats or brown rice, and healthy fats such as olive oil supports overall wellness and weight management, both of which are friendly to your joints.
Low-fat dairy products deserve special mention because they have been associated with lower uric acid levels. A cup of low-fat milk or a serving of yogurt can be a smart daily choice for many people, unless dairy does not agree with you. Including one or two servings of low-fat dairy most days is a simple, practical step you can try.
What to limit to help prevent flares
Certain drinks and foods can nudge uric acid upward. Sugary beverages sweetened with high-fructose corn syrup are a common trigger, and cutting them back often brings noticeable benefits. Alcohol can also raise uric acid and make flares more likely, especially beer and spirits. If you drink alcohol, consider smaller amounts and more alcohol-free days, and discuss with your clinician what is right for you based on your health history and medications.
Large, heavy meals can sometimes bring on a flare, especially after periods of dieting or dehydration. Gentle balance is your friend. Regular meals with sensible portions are easier on your body than big feasts or crash diets. Sudden, extreme dieting can briefly raise uric acid and should be avoided. Slow, steady changes are more effective and kinder to your joints.
Weight, movement, and joint comfort
If you are carrying extra weight, even a modest loss over time can lower uric acid and reduce pressure on your joints. There is no need to aim for a dramatic change. Losing just a few pounds over several months can make walking easier and lower your risk of flares. Pairing a thoughtful eating plan with gentle activity can help. Walking, swimming, cycling on a stationary bike, or water aerobics are excellent low-impact choices that are easy on the joints. During a flare, rest the affected joint, then gradually return to activity as the pain settles.
Strength and flexibility also matter. Simple stretching and light strength exercises support the muscles that protect your joints. If you are unsure where to start, a physical therapist can create a plan tailored to your comfort and abilities. Many people in their fifties and sixties find that a few short sessions each week make daily tasks feel easier.
Medications and checkups that support long-term health
Some prescription medicines raise uric acid. Water pills used for blood pressure or swelling, certain immune-suppressing drugs, and high-dose niacin are examples. Low-dose aspirin can raise uric acid slightly but is often important for heart health. Never stop a prescribed medication on your own. Instead, ask your clinician if there are alternatives that fit your needs, or if an adjustment could help while still protecting your heart and blood pressure.
For many people with repeated flares, long-term uric acid–lowering medications such as allopurinol or febuxostat are the most effective way to dissolve crystals and prevent new ones. These medicines work best when taken consistently and monitored with simple blood tests. Your clinician may set a uric acid target, often below 6 mg/dL, to help crystals gradually disappear. When starting these medications, providers sometimes add a short-term anti-inflammatory plan to prevent early flares. Staying the course is important; over time, most people notice fewer flares and better joint comfort.
Kidney health and uric acid
Your kidneys are your main partners in clearing uric acid. Keeping blood pressure, blood sugar, and cholesterol in good ranges supports kidney function. Regular checkups and lab tests help catch concerns early. If you have a history of kidney stones, let your clinician know, because certain steps can lower the chance of uric acid stones. Hydration, balanced eating, and medication choices can all be tailored to protect your kidneys while managing gout.
Cherries, vitamin C, coffee, and other common questions
Many people ask about cherries, vitamin C, and coffee. Studies suggest that cherries and cherry extracts may help reduce the chance of a flare for some people, likely due to their anti-inflammatory compounds. They are not a cure, but including cherries as part of a healthy eating plan is reasonable if you enjoy them. Vitamin C from foods such as citrus fruits, strawberries, bell peppers, and broccoli may gently lower uric acid, but talk with your clinician before taking supplements, especially if you have kidney issues or take multiple medications.
Moderate coffee intake has been linked with a lower risk of gout in some studies, though coffee is not right for everyone. If you already drink coffee and tolerate it well, there is no clear reason to stop for gout specifically. If you do not drink coffee, there is no need to start for this reason alone. Above all, avoid making big changes without checking how they fit with your overall health plan.
Myths, quick fixes, and staying safe
It is easy to find bold promises online about “flushing out” uric acid overnight with a special drink, baking soda, or a harsh cleanse. Be cautious. Some of these ideas can be risky, especially if you have high blood pressure, heart disease, or kidney concerns. Others simply do not work. Your safest path is a steady routine built on hydration, balanced meals, gentle activity, and medical guidance when needed. These steps may not sound flashy, but they are proven and they protect your long-term joint health.
Supplements can interact with medications or stress the kidneys. If you are curious about a supplement, write down the name and bring it to your next appointment. A short conversation with your clinician or pharmacist can help you avoid unwanted side effects and choose options that truly help.
A simple day-by-day approach
Imagine a typical day built around joint comfort and lower uric acid. You start your morning with a glass of water and a balanced breakfast that might include oatmeal topped with berries and a spoonful of yogurt. Mid-morning, you take a short walk or do a few gentle stretches. At lunch, you choose a colorful salad with grilled chicken or tofu, a slice of whole-grain bread, and another glass of water. In the afternoon, you pause to sip water again and, if you enjoy coffee and it suits your health, a small cup. Dinner is satisfying but not heavy, perhaps salmon or a bean-and-vegetable stew, along with steamed greens and brown rice. If you drink alcohol, you skip it tonight or keep it minimal.
On this kind of day, your joints get steady support. You are not avoiding everything you enjoy, just making small choices that add up. Over weeks and months, these patterns can help lower uric acid, protect your kidneys, and reduce the chance of gout flares. If you also take a prescribed medicine to lower uric acid, you set a reminder and take it at the same time each day, then follow up with your clinician for simple blood tests to track progress.
When to seek medical care
If you are not sure whether you have gout, or if a joint becomes very painful, hot, and swollen, contact your clinician. Sometimes an infection in a joint can look like gout and needs urgent treatment. If you have a fever along with joint pain, new severe pain in your back or side, trouble passing urine, or blood in your urine, seek medical care promptly. These symptoms can suggest other conditions, such as a kidney stone or an infection, that should not wait.
Putting it all together for steady relief
While there is no instant way to erase uric acid crystals, you can take confident steps today that lead to real relief. During a flare, rest the joint, use cool compresses, and talk with your clinician about anti-inflammatory treatments that fit your health history. Day by day, support your body with water, balanced meals that go easy on high-purine foods and sugary drinks, and gentle movement that feels good. If you need a long-term uric acid–lowering medicine, take it consistently and celebrate the progress you make along the way.
Your joints carry you through life’s most meaningful moments, from walks with friends to family gatherings and quiet times at home. With a practical plan and the right support, you can reduce uric acid, calm inflammation, and look forward to more comfortable days. If you have questions, bring them to your next visit. A few small changes, made steadily, can add up to big improvements in how you feel and move.