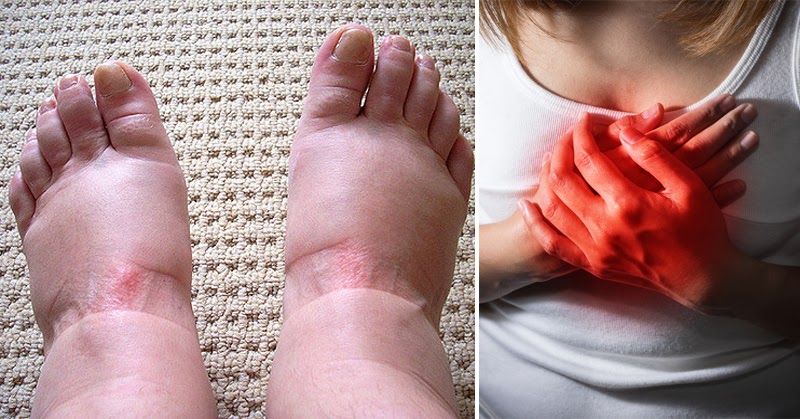
Swollen feet are something many people notice from time to time, especially as we get older. Maybe your shoes feel tight at the end of the day, or you see a little puffiness around your ankles after a long car ride. Often, that kind of swelling settles down with rest, elevation, and a good night’s sleep. But sometimes swelling is your body’s way of waving a red flag, letting you know something else needs attention.
This friendly guide is here to help you understand the difference between everyday swelling and warning signs you shouldn’t ignore. You will learn what to watch for, when to call your doctor, and simple steps that can bring relief. If you ever feel unsure, trust your instincts. It is always okay to ask a healthcare professional for advice.
Before we dive in, a quick note on what swelling is. Doctors call it edema, and it happens when fluid builds up in the tissues. Gravity tends to pull that fluid toward our feet and ankles, so that’s where we often see it first. The cause can be minor, like heat, salty foods, or standing still for too long. But it can also point to issues with circulation, the heart, kidneys, liver, or even an infection or injury. Learning the warning signs can help you act early and feel your best.
Deep vein thrombosis
One of the most urgent causes of one-sided leg or foot swelling is a blood clot in a deep vein, called a deep vein thrombosis, or DVT. A DVT can block blood from flowing back to your heart, which leads to swelling, warmth, and tenderness in the affected leg. The swelling is usually more noticeable on just one side and may not improve much with rest or elevation.
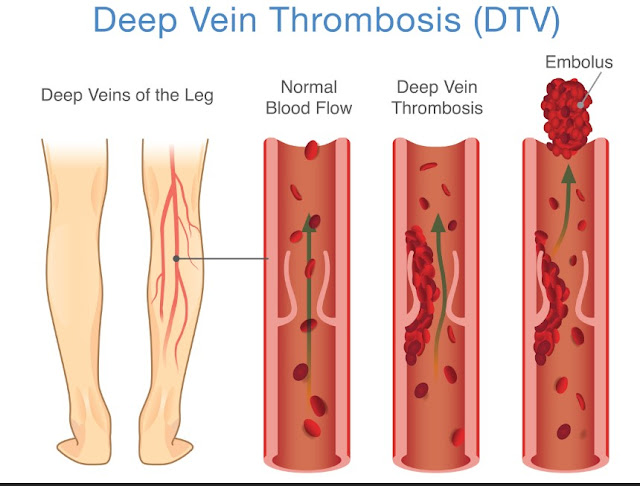
Common warning signs of a DVT include new swelling in one foot, ankle, or calf; warmth and redness over the area; and aching or cramping pain that may feel worse when you stand or walk. Some people notice the skin looks tight or shiny compared with the other leg. It can start after long travel, a recent surgery or hospital stay, cancer treatment, or periods of being less active.
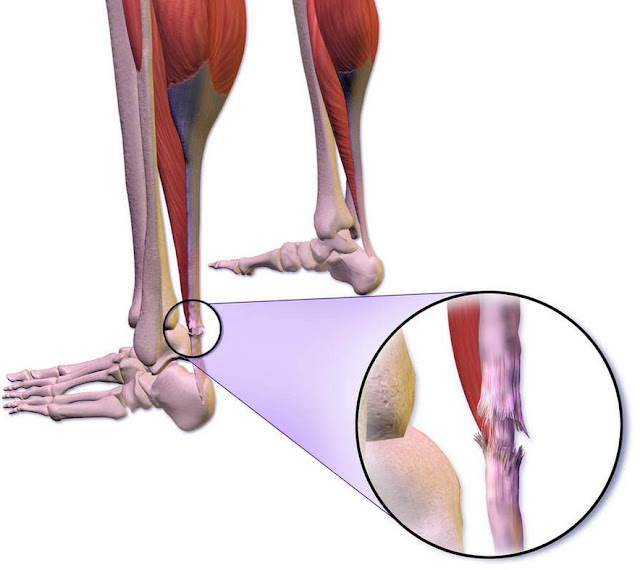
If you suspect a DVT, do not massage the leg or try to “walk it off.” A clot can break loose and travel to the lungs, causing a life-threatening emergency called a pulmonary embolism. Call your doctor right away or seek urgent care. If you also have sudden shortness of breath, chest pain, or feel faint, call emergency services immediately.
Doctors usually diagnose a DVT with a quick, painless ultrasound of the leg. Treatment often includes blood thinners to stop the clot from growing and to prevent new ones from forming. The sooner a DVT is found and treated, the lower the risk of serious complications.

Risk grows with age and is higher if you have had a prior clot, certain genetic clotting conditions, cancer, recent major surgery, hormone therapy, or long stretches of sitting still, such as on flights or car trips. Staying hydrated, taking walking breaks, and gently moving your ankles while seated can help lower risk, but they do not replace medical care if symptoms appear.

Compression socks can be helpful for circulation in some people, but do not put them on a leg you think has a new clot unless a clinician tells you to. Gentle elevation of the leg above heart level can ease discomfort while you wait for care, but the priority is to be seen promptly.
Remember, DVT is one urgent reason for swollen feet, but not the only one. The key is noticing what else is happening in your body and how quickly the swelling appeared. The following sections walk you through other important warning signs and what they may mean.
As you read through the signs below, pay attention to whether your swelling is on one side or both, whether it improves after a night’s rest, and whether you have symptoms like shortness of breath, fever, skin changes, or pain. These clues help narrow down the cause and guide the next steps.
If your swelling came on suddenly or is getting worse quickly, it is safer to be checked sooner rather than later. When in doubt, lean toward a phone call or visit. Peace of mind is valuable, and early care can prevent bigger problems.

Swelling with shortness of breath or needing extra pillows to sleep
If both feet and ankles are puffy, especially by evening, and you also feel short of breath or notice you need more pillows to sleep comfortably, your heart could be asking for help. When the heart has trouble keeping up, fluid can back up in the legs and lungs. You might also see weight creep up over a few days from fluid retention, or notice socks leaving deeper marks than usual.
This combination of swelling and breathlessness deserves prompt attention, particularly if it is new or worsening. Simple changes like lowering salt, taking prescribed water pills as directed, and elevating your legs can help, but a checkup is important to adjust treatment and rule out anything urgent. Seek immediate care if breathing becomes suddenly worse, you have chest pain, or you feel lightheaded.
Swelling with puffy eyelids in the morning and changes in urination
When your kidneys are not filtering fluid effectively, you may notice swelling in both feet and ankles along with puffiness around the eyes when you wake up. Urine may look foamy or you may be going less often. Some people also notice fatigue, a poor appetite, or higher blood pressure.
Kidney-related swelling often lingers throughout the day and may not improve much overnight. Blood and urine tests can check kidney function and protein levels. If you take pain relievers like NSAIDs, certain blood pressure medicines, or other medications, ask your doctor whether they could be affecting your kidneys. Do not stop prescribed medicines on your own, but do bring a full list to your appointment so your clinician can review them with you.
Swelling with a full, tender abdomen or yellow-tinged skin
Liver problems can lead to fluid buildup in the belly and legs. You may notice the waistband of your pants feels tight, your appetite is down, or the skin and whites of your eyes look slightly yellow. The swelling is usually in both legs and may be accompanied by easy bruising or feeling more tired than usual.
If these signs sound familiar, it is wise to schedule a checkup. Your doctor can evaluate your liver with blood tests and, if needed, imaging. Lifestyle steps like limiting alcohol, maintaining a healthy weight, and getting vaccinated for hepatitis can support liver health, but medical guidance is key if swelling is present.
Red, hot, and painful swelling with or without fever
When the skin of the foot or lower leg becomes red, warm, swollen, and tender to the touch, an infection called cellulitis may be the cause. Sometimes there is a small cut, cracked skin, or a fungal infection between the toes that opens the door for bacteria to enter. People with diabetes, circulation problems, or lymphedema are at higher risk.
Cellulitis requires medical treatment, usually antibiotics. Do not delay if you see red streaks moving up your leg, you have a fever or chills, or the pain is quickly worsening. While you wait for care, keep the leg comfortably elevated and avoid squeezing it with tight socks or shoes. Good skin care and nail care are helpful prevention tools once the infection clears.
Sudden, intense pain in a toe or foot with warmth and redness
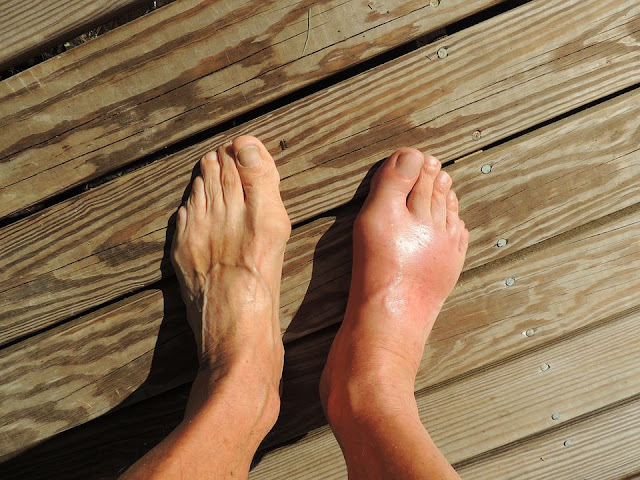
Gout, a form of arthritis, can cause dramatic swelling and pain, often in the big toe. It may come on overnight and feel like the joint is on fire, with the skin looking shiny and red. A gout flare can follow a rich meal, dehydration, illness, or certain medications. While the pain is striking, the good news is that gout is very treatable.
Your clinician can confirm gout and recommend medicines that calm the flare and reduce future attacks. Drinking water, resting the joint, and avoiding alcohol during a flare can help. Over time, managing risk factors and, when appropriate, using uric-acid–lowering therapy can cut down on repeat episodes.
New swelling after a twist, fall, or misstep with trouble bearing weight
Injuries like sprains, strains, or fractures often cause swelling, bruising, and tenderness around the foot or ankle. If you cannot put weight on the foot, the pain is severe, or the shape looks unusual, it is best to be evaluated quickly to check for a break. An X-ray or other imaging may be needed.
Until you can be seen, rest the foot, keep it gently elevated above your heart if possible, and apply a cold pack wrapped in a thin towel for short periods to reduce discomfort. Avoid heat or deep massage over a fresh injury, and let a clinician guide when and how to return to activity safely.
Swelling with numbness, color changes, or cramping when you walk
If your feet feel cold or look pale or bluish, or you notice cramping in your calves when walking that improves with rest, circulation may be reduced. This can be a sign of peripheral artery disease, where arteries have narrowed and blood flow is limited. Diabetes and smoking raise the risk, as do high cholesterol and high blood pressure.
In other cases, numbness and tingling point more to nerve issues, such as diabetic neuropathy or a pinched nerve in the back. Either way, new swelling with these symptoms deserves a checkup. Depending on the cause, treatments might include walking programs, medicines, smoking cessation support, and, in some cases, procedures to improve blood flow.
Swelling that does not go down overnight and leaves little or no pit
When swelling lingers day after day and the skin feels firm or thickened, lymph fluid may be backing up, a condition called lymphedema. It often begins around the toes or top of the foot and can gradually spread upward. In contrast to simple fluid retention, pressing a finger into the skin may leave little or no indentation. Lymphedema can follow surgery, radiation, infection, or it can develop on its own.
Chronic venous insufficiency, where leg veins have trouble sending blood back to the heart, can also cause long-lasting swelling, skin discoloration, and aching. Elevation, movement, and properly fitted compression garments can help, but it is smart to have a clinician take a look to tailor care and protect the skin.
General swelling that worsens by evening and improves with leg elevation
Not every warning sign points to an emergency, but persistent, bothersome swelling that returns most days is still worth discussing with your healthcare team. You may notice sock marks by afternoon, and your shoes might feel tighter after standing or sitting for long stretches. This pattern can reflect fluid retention from medications, heat, salt intake, or vein-related issues.
Keep a simple diary for a week noting when swelling is better or worse, how much time you spend sitting or standing, any new medicines, and what helps. Bring those notes to your next appointment. Useful changes often include taking seated breaks to move your ankles, propping your feet up when you can, limiting salty foods, staying well hydrated, and wearing supportive footwear. A clinician can guide whether compression socks are right for you and at what strength.
What you can do right now to feel better
When swelling is mild and you do not have red-flag symptoms like chest pain, severe shortness of breath, fever, or one-sided sudden swelling, a few home steps can bring relief. Rest with your feet raised on pillows so that your ankles are above your heart for 15 to 20 minutes a few times a day. Point and flex your ankles and wiggle your toes now and then to keep blood moving.
Drink water regularly throughout the day unless your doctor has told you to limit fluids. Choose meals lower in salt, since salt makes the body hold on to fluid. If you sit for long periods, such as at a computer or on a long drive, take brief walking breaks or march in place to keep circulation active. Supportive, well-fitted shoes can also make a meaningful difference.
Compression socks can help many people, but they are not for everyone. If you have poor circulation, open sores, or think you might have a blood clot, get medical advice first. When they are appropriate, a proper fit and the right compression level make them more comfortable and more effective.
How your clinician figures out the cause
To pinpoint why your feet are swelling, your clinician will look at the whole picture: your history, what the swelling looks and feels like, and any other symptoms. They may check your heart, lungs, belly, skin, and pulses in your feet. Depending on what they find, tests might include an ultrasound to check for a clot, an X-ray if injury is suspected, and blood or urine tests to see how your heart, kidneys, liver, and thyroid are doing.
Knowing the cause leads to tailored treatment. That might mean medicines to remove extra fluid, treat infection, ease gout, or dissolve clots; it might mean physical therapy, compression therapy, or specific lifestyle changes. The goal is always the same: to protect your health and help you feel comfortable on your feet again.
Prevention pointers for calmer feet
A few everyday habits can reduce the chances of troublesome swelling. Build gentle movement into your day, even if it is five minutes each hour. Keep your legs uncrossed when sitting, and try not to stand completely still for long periods. Maintain a balanced diet with enough protein and less added salt, and aim for a steady, healthy weight.
If you take medicines that may cause swelling, such as certain blood pressure pills, hormones, or anti-inflammatory drugs, ask your doctor whether adjustments could help. Care for your skin by moisturizing daily and treating small cuts promptly. And if travel is on your calendar, plan stretch breaks and ankle pumps on the go to keep circulation humming.
The bottom line
Swollen feet are common, but they are not something to brush off when they come with warning signs. Seek urgent help for one-sided swelling with pain and warmth, sudden shortness of breath or chest pain, fever with red and tender skin, or severe pain after an injury. Make a prompt appointment if swelling is new, persistent, or paired with symptoms like breathlessness at night, changes in urination, a tight and swollen belly, numbness or color changes in the feet, or swelling that does not improve by morning.
Your body is wise, and swelling is often its way of asking for a closer look. With timely attention and a few smart daily steps, most people can get to the bottom of what is going on and get back to moving comfortably. If you are ever unsure, a quick call to your healthcare team is a caring step for yourself—today and every day.