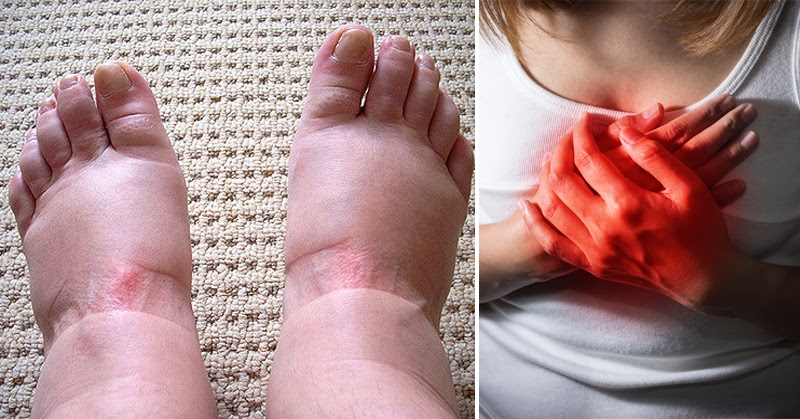
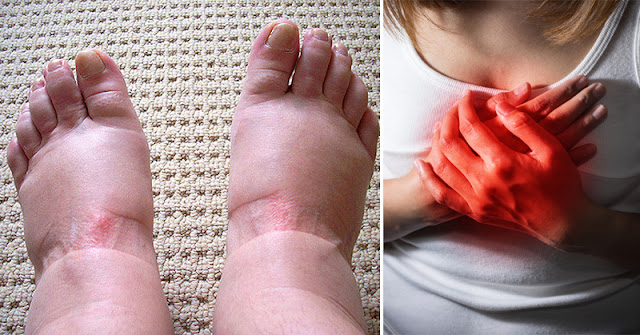
Swollen feet are common, especially as we get older. A long day on your feet, a salty meal, warm weather, or sitting too long on a car or plane ride can all make your shoes feel tight by evening. Most of the time, this kind of swelling eases with rest, leg elevation, and a good night’s sleep. Still, there are times when swollen feet are your body’s way of waving a red flag. Knowing the difference can help you act quickly, protect your health, and feel better sooner.
If you are between the ages of 45 and 65, you may be noticing changes in circulation, joint comfort, and how your body handles fluids. Hormones, blood pressure, heart and kidney health, and even common medications can all influence swelling. That is why it helps to pay attention not only to the swelling itself but also to the symptoms that show up alongside it. Certain patterns—like swelling that appears suddenly, affects just one foot, or comes with pain, shortness of breath, or skin changes—deserve prompt attention.
Below you will find the most important warning signs to watch for. If you recognize any of these in yourself or someone you love, contacting a healthcare professional is the safest next step. And if you notice severe symptoms—such as chest discomfort, trouble breathing, or a cold, pale foot—do not wait. Seek urgent care right away.
Deep vein thrombosis
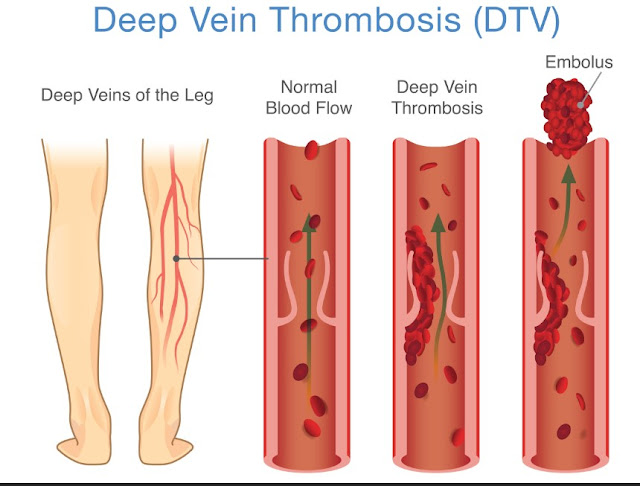
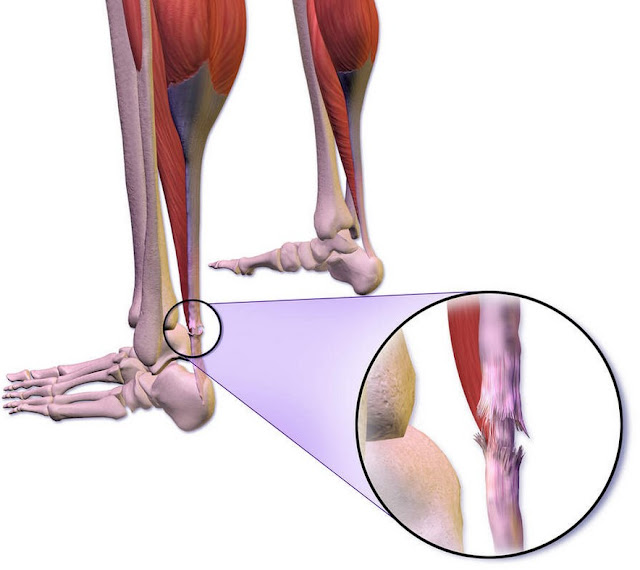

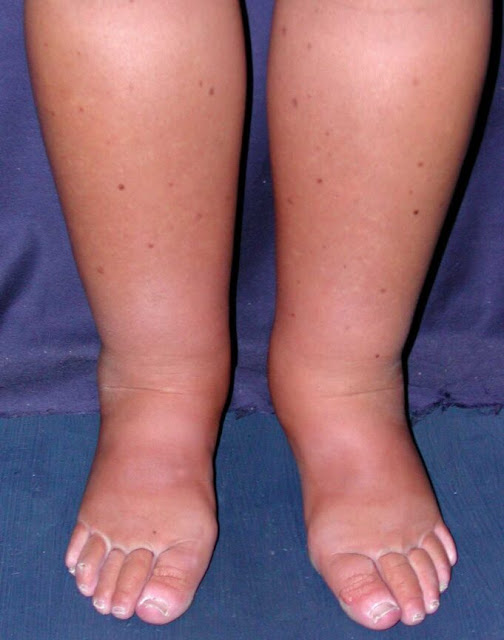

One of the most serious explanations for sudden swelling in a single foot or calf is a deep vein thrombosis, often called a DVT. This is a blood clot that forms in a deep vein, usually in the lower leg. Because the clot blocks normal blood flow, fluid backs up and the leg becomes puffy. The area may feel tender, heavy, or warm, and the skin can look red or slightly blue. Some people notice the discomfort most when they stand or walk, or they feel a tight, cramping sensation in the calf.
A DVT needs medical attention right away because part of the clot can travel to the lungs and cause a life-threatening condition called a pulmonary embolism. Call emergency services if swelling comes with chest pain, sudden shortness of breath, coughing up blood, a racing heartbeat, or feeling faint. Even without those symptoms, if one leg is clearly larger than the other and you have pain or warmth, it is important to be seen promptly. A quick ultrasound can confirm the diagnosis, and treatment can protect you from serious complications.
DVTs are more likely after long travel or bed rest, recent surgery, a leg injury, or if you have certain medical conditions. Smoking, being overweight, taking hormone therapy, and a family history of clots can also raise risk. If you often sit for long periods, taking short walking breaks, flexing your ankles, and staying well hydrated can help keep blood moving.
Sudden swelling in one foot or ankle
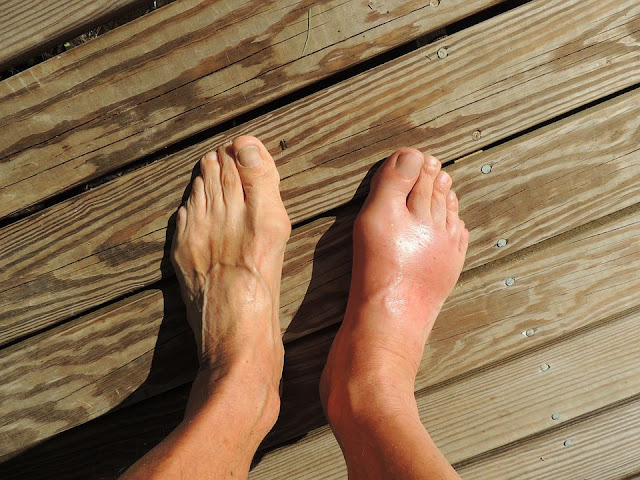
Most everyday ankle swelling is fairly even in both feet and builds gradually as the day goes on. When swelling appears suddenly in just one foot or ankle, especially within a few hours, it deserves attention. A single swollen foot can signal a blood clot, a torn tendon, an ankle sprain, or even a small fracture you did not realize you had. Sometimes people will notice their shoe on one side no longer fits while the other still does, or they feel a tight band sensation around one ankle.
If you have recently been on a long car or plane ride, had an illness that kept you in bed, or started using a walking boot or cast, call your clinician the same day to ask whether you should be examined or go to urgent care. The key point is the mismatch between your two legs. When one side is clearly more swollen, it is safer to check for a clot or injury sooner rather than later.
Red, hot, or streaked skin over the swollen area
Swelling that comes with warmth, redness, or red streaks running upward on the skin can be a sign of an infection in the skin and soft tissue, known as cellulitis. This usually happens when bacteria enter through a small cut, blister, or fungal crack between the toes. The infected area becomes hot and tender, and you might also have a fever or chills. Cellulitis can spread quickly, which is why prompt treatment matters.
People with diabetes, circulation problems, or a history of skin infections should be especially cautious. If the skin looks shiny, is painful to touch, and you notice spreading redness, call your doctor or go to urgent care. Antibiotics can usually settle the infection within a few days, and treating it early helps you avoid complications and reduces the chance of lingering swelling.
Weeping blisters, open sores, or skin that will not heal
When the skin on the feet and ankles stays puffy for a long time, it stretches and becomes fragile. You may see fluid-filled blisters, oozing areas, or small ulcers that do not close. These changes are warning signs that the skin’s protective barrier is breaking down. Open spots are an open door for infection, and they can be slow to heal if swelling and poor circulation continue.
If you notice any open area, keep it clean and dry, protect it with a simple bandage, and contact your clinician for advice. Wearing well-fitted shoes and socks, moisturizing dry skin, and avoiding walking barefoot can help protect vulnerable areas. When swelling is controlled, the skin can repair itself more easily.
Swelling with shortness of breath or chest pressure
Swollen feet paired with breathlessness, a cough that worsens when you lie down, or a feeling of pressure or heaviness in the chest may point to fluid overload related to the heart. When the heart does not pump as efficiently as it should, fluid can build up in the legs by day and shift toward the lungs at night. Some people notice they need extra pillows to sleep or they wake up gasping for air. Weight can creep up by several pounds over a few days as the body holds onto salt and water.
If this description sounds familiar, it is wise to speak with your healthcare provider soon. A simple exam, blood tests, and possibly an echocardiogram can clarify what is going on. The good news is that with the right plan—adjusting medications, reducing sodium, and staying active within your comfort range—many people feel significantly better and see the swelling decrease.
Puffy eyes or foamy urine along with foot swelling
When swelling shows up not just in the feet but also around the eyes, especially first thing in the morning, the kidneys may be involved. The kidneys’ job is to balance fluids and filter waste. If they are not working well, fluid can accumulate and protein can leak into the urine, causing it to look unusually foamy or bubbly. You might also notice that your rings feel tight or you need to loosen your watch band.
These are clues to contact your clinician for a check-up. Simple urine and blood tests can evaluate kidney function. Managing blood pressure, blood sugar, and salt intake can go a long way toward protecting the kidneys. Catching kidney changes early gives you more options and helps prevent more serious problems later.
Yellowing skin, a tight belly, or easy bruising with swollen feet
The liver also plays an important role in fluid balance. When it is struggling, the body can hold onto fluid in the legs and abdomen. Warning signs linked to the liver include yellowing of the skin or eyes, a sense of fullness or tightness in the stomach, and bruising more easily than before. You may find that socks leave deeper marks on your ankles and your pants feel snugger around the waist even if your weight has not changed much.
If you see these patterns, it is worth scheduling a visit with your healthcare provider. Blood tests and an ultrasound can check on liver health. Limiting alcohol, maintaining a healthy weight, and following your clinician’s guidance can often ease swelling and support your liver’s ability to heal.
A cold, pale, or numb foot
Swelling usually points to extra fluid, but a foot that turns cold, pale, or bluish and becomes numb or very painful is a different kind of emergency. These symptoms suggest that blood is not reaching the foot properly. This can happen if an artery is blocked or severely narrowed, which reduces oxygen to the tissues. In addition to color changes, you may notice the foot becomes weak, you cannot feel your toes well, or pain worsens when you prop the leg up.
This situation is urgent because tissues need a constant supply of oxygenated blood. If these symptoms appear suddenly, seek emergency care. Even if they come and go, mention them to your doctor right away. Early treatment can restore circulation and protect your foot from damage.
Swelling that begins after a new medication
Some very common medications can cause fluid to pool in the feet and ankles. Blood pressure drugs called calcium channel blockers, certain diabetes medicines, hormone therapy, steroids, and even over-the-counter pain relievers can sometimes make swelling worse. You might notice that your socks leave deeper imprints or your shoes feel tight within a few days to a few weeks of starting something new.
Do not stop a prescribed medication on your own, but do call your clinician or pharmacist to discuss what you are seeing. Often there are alternatives or small adjustments that can help. Keeping a simple note of when the swelling started, what time of day it is worst, and any other changes you have noticed gives your care team helpful clues to tailor a solution for you.
How to care for swollen feet at home and when to call
For everyday swelling from standing or sitting, try resting with your feet above the level of your heart for 20 to 30 minutes a few times a day. Gentle ankle circles and pumping your feet up and down help move fluid along. Staying well hydrated may sound counterintuitive, but it supports healthy circulation and prevents your body from clinging to salt. Comfortable, supportive shoes with a roomy toe box and soft socks that do not dig into the skin can make a big difference by day’s end.
Many people also find compression socks helpful. If you have not used them before, ask your healthcare provider which strength and style are right for you. They are designed to support your veins and encourage blood to return to the heart. Put them on in the morning when swelling is typically lowest for the best effect. If compression causes pain, numbness, or skin irritation, remove them and check in with your clinician.
Most importantly, listen to your body’s warning signs. Seek emergency care for sudden one-sided leg swelling with pain and warmth, swelling paired with chest discomfort or shortness of breath, a cold or blue foot, or symptoms that come on quickly after an injury. Arrange a prompt clinic visit if swelling is new, persistent, or accompanied by redness, fever, weeping blisters, changes in skin color, weight gain over a few days, or if it begins after a new medication.
Swollen feet do not have to be a mystery. By noticing the patterns, acting on the red flags, and partnering with your healthcare team, you can uncover the cause, protect your health, and get back to comfortable, confident steps day after day.